A Smart Choice For Patients
PATIENTS-GENERALLY SPEAKING
Protein requirements may be significantly increased when you suffer serious injuries and/or illnesses. This is especially true when you are facing an operation. The ability to heal surgical wounds and fight infection is of paramount importance. Frankly, returning to wellness depends on it.
Terms you are going to see a lot of in my writings are Protein Energy Malnutrition, PEM, which is also called Protein Calorie Malnutrition, or PCM. The two are interchangeable. Put simply, you are not getting enough protein to satisfy your body’s nutritional needs.
Malabsorption and altered metabolism may also be possible contributors. But, for the most part, eating sufficient amounts of protein will help solve this particular problem.
The amount of protein you need should be determined by your personal case and caregivers. Dr. Steve’s Nutri Snax simply offers a choice of protein to help you meet your Personal Protein RDA and beyond if deemed necessary.
There is a predominance of PCM among patients. PCM leads to increased complications, morbidity, mortality, prolonged hospital stays, hospital readmissions, and healthcare costs; physical, mental, and financial. As a surgeon, I consider protein stability to be a critical first step in inpatient care. The following is a partial list of clinical settings where Dr. Steve’s Nutri Snax may be used to help these patient groups meet their protein needs: Pre/Post-operative (Surgical), Chronic Wound Care, Diabetes/Prediabetes, Renal Failure/Dialysis, Celiac Disease/Non-Celiac Gluten Sensitivity (Gluten-Free, GF), Anorexia/Bulimia, Cardiovascular Disease, Chronic Obstructive Pulmonary Disease (COPD), HIV/AIDS and Cancer.
In fact, the latest surgical literature is beginning to address the preoperative and postoperative (4-8 weeks after surgery), status of surgical patients in regards to exercise and increased nutritional needs, especially concerning protein. This structured conditioning program has been termed “prehabilitation.” Prehabilitation applies to patients facing major surgery, but it is also being employed in cancer patients undergoing chemotherapy and radiation treatments. Acknowledging and addressing these needs may be of great benefit. Some research is suggesting prehabilitation protein intake should be 1.2-1.5 grams of protein/kg of body weight/day to meet the body’s increased demands. Please recall our 160-pound person with an RDA of 64 grams of protein. Prehabilitation recommendations in this particular case now range from 96 to 120 grams of protein per day (80 x 1.2 and 1.5, respectively). This is a new frontier in surgical care, and Dr. Steve’s Nutri Snax may help patients achieve their nutritional goals to satisfy increased perioperative protein requirements. To reiterate, your personal protein needs should be determined by your own caregiving team without exception.
CANCER
CANCER - To me, this group of patients tops the list concerning their urgent need for protein. Although this product is meant for anyone to enjoy, my clinical/surgical experience regarding taking care of cancer patients is the main reason I created Dr. Steve’s Nutri Snax.
All these patient groups may experience some degree of gastrointestinal (G-I), dysfunction, and this is especially true of cancer patients. This is because numerous forces act against the human body when it comes to eating, drinking, and digesting nutrients under stressful conditions. For example, pain, inactivity, surgery, pain medication (think opioids), radiation, chemotherapy, and the disease itself are causative factors, as bodily functions may grind to a halt. As a solution, patients are often asked to drink liquids to help them meet their nutritional needs, protein included. While liquid forms of nutrition may certainly have their place, the problem is they often add an excessive volume load to the compromised G-I tract. For this and other reasons, liquid nutrition is frequently poorly tolerated, which may lead to nausea, vomiting and/or diarrhea. As a result, this may cause serious loss of electrolytes (especially sodium), which must be replaced. These aforementioned patient groups may require extra protein to heal properly, but in my opinion; the most-dramatic need is seen in cancer patients.
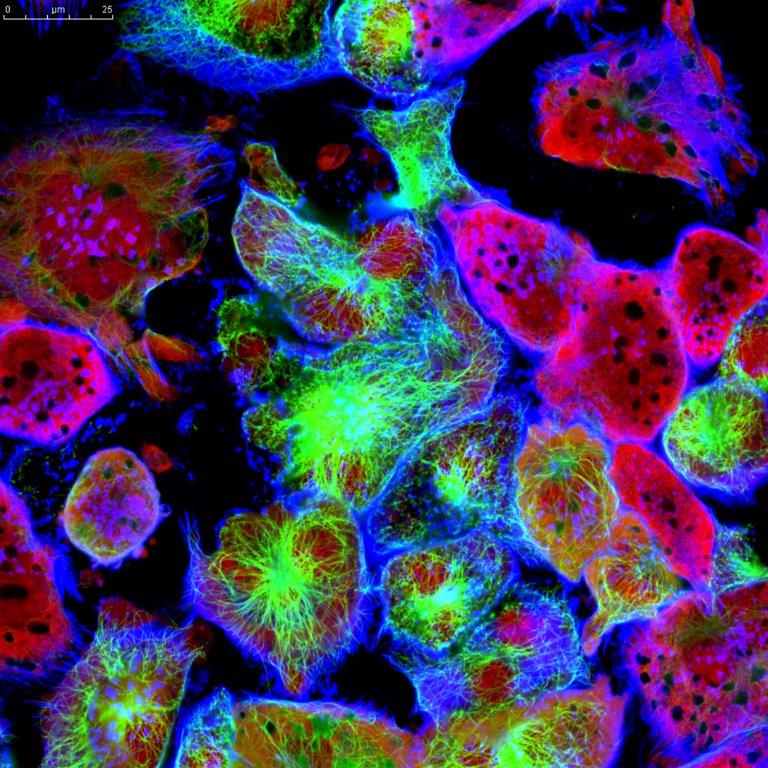
"Tumor cells under microscope labeled with fluorescent molecules."
CANCER PATIENTS & PROTEIN CALORIE MALNUTRITION
A very significant number of my patients had cancer. My mom, dad and two of my uncles had cancer. All of us have been affected by this disease in some way. Dr. Steve’s Nutri Snax may help all patient groups, especially those stricken with cancer, meet their increased protein needs. From the National Cancer Institute: “The loss of body protein produces the complications of malnutrition which can lead to progressive muscle wasting, weakness, and debilitation as protein synthesis is decreased and lean body muscle mass is lost, possibly leading to death.” Any loss of body protein is detrimental. If nothing else, this product offers patients a choice of protein they never had before in the form of a crunchy snack, which provides a minimum of 13-15 grams of protein per one-ounce bag (depending on the flavor).
Protein Calorie Malnutrition must be brought to the forefront as it relates to cancer patients. They often face a combination of surgery, radiation treatments or chemotherapy, sometimes all three. Using chemotherapy as an example; PCM is associated with increased side effects, toxicity, and treatment delays. In addition to chemotherapy, certain specific problems may also arise during and after radiation treatments. Please visit the blog I wrote for The Leukemia & Lymphoma Society/PearlPoint Cancer Support: The Importance of Protein During Radiation: https://pearlpoint.org/importance-protein-during-radiation/. To return to wellness, patients not only have to survive their disease; they have to survive their treatment. To have the best chance for success, patients need to be protein stable. Unfortunately, we are falling way short.
In fact, the National Cancer Institute in Cancer Care-Health Professional Version-2017 stated the following: “Protein Calorie Malnutrition is the most common secondary diagnosis in individuals diagnosed with cancer. Malnutrition is a common problem in cancer patients that has been recognized as an important component of adverse outcomes, including increased morbidity, mortality and decreased quality of life,” or QoL. In simple terms, PCM increases human suffering and certainly may lead to death. If a patient can’t eat, it drastically affects their QoL. We, as physicians and caregivers, should never underestimate just how important it is for patients to eat solid food and for their families to see them eat. Subjective, intangible components should never be overlooked. It is important to recognize Quality of Life is not just a term meant for patients. It also applies to everyone involved; family members, nurses, dietitians, therapists, and doctors. We are part of a team dedicated to all aspects of patient care. If the patient is not doing well, then we are not doing well.
It is important to know the cancer care-giving and scientific communities now, more than ever, are recognizing just how important it is for cancer patients to consume extra amounts of protein. The literature in this area is now suggesting cancer patients need to eat 1.0-2.5 grams of protein/kilogram of body weight/day. There are many variables to consider, such as cell type, tumor location, involved treatments, etc., but in general, this is a recommended range (from anorexia to cachexia). To reiterate, each case is formulated on an individual basis according to the treatment plan established by your doctor and caregiving team. To put this in perspective, for the 160-pound person, the RDA was 64 grams of protein. For the 160-pound cancer patient, the protein need has significantly increased to a range from 80-200 grams of protein per day in order to meet these new demands secondary not only to the disease but also the treatment, as both may contribute to the development of PCM. Once that protein requirement has been accurately determined by caregivers, the patient needs to do everything in their power to meet that number.
This is why Dr. Steve’s Nutri Snax is placed in one-ounce packaging. It makes it easy to incorporate into the daily routine as it relates to both eating and keeping an accurate record of how many grams of protein are actually consumed that day. This will help patients meet their personal protein RDA and any additional protein needs if required. Now you know why it is very important to know the number of grams of protein a cancer patient is eating, or not eating every day, and why Protein Calorie Malnutrition is so prevalent among this group of patients. My goal is to solve this problem. As a reminder, A BAG A DAY FOR YOUR RDA!
CANCER PATIENT RESULTS-SARAH CANNON CANCER RESEARCH INSTITUTE
In my original research with this project, samples of Dr. Steve’s Nutri Snax were sent to various cancer centers across the country. Most of our work, however was performed at Sarah Cannon Cancer Center, SCCC and Sarah Cannon Cancer Research Institute, SCCRI. During our work with SCCC/SCCRI, we discovered many notable findings: Not one patient became ill after consuming our product. Patients not only tolerated the product, they enjoyed it. Also, patients told us liquid forms of nutrition “dehumanize.” The simple act of chewing solid food was considered a very important part of their quality of life. If for whatever reason, patients could not chew, they simply dissolved this product under their tongues accompanied only by sips of water, thus avoiding gastrointestinal problems often seen with liquid forms of nutrition.
Please note the following comments from Dr. Tony Greco, M.D., Co-Founder of Sarah Cannon Cancer Research Institute:
"As you know, cancer is a very heterogeneous group of diseases and the degree of illness patients suffer is extremely variable. In any regard, the degree of Protein Calorie Malnutrition is a major factor. I think your product is an excellent source of protein, and the patients have liked the product. Problems with nausea and vomiting did not occur. The different flavors offer an advantage. Overall, I think a solid form of protein supplementation in a concentrated form such as your product offers an important advantage for some patients who tend to fill up quickly on liquid forms of protein supplementation. I also think some patients are more likely to ‘snack’ on your product, much like ‘corn chips’ or other popular snack foods. In summary, your product is liked and convenient. It is easy to administer and seems very tolerable and has a very substantial protein content.”
Dr. Greco is a co-founder of Sarah Cannon Cancer Research Institute. He earned a fellowship in medical oncology from the National Cancer Institute. Dr. Greco also was the Director of the Vanderbilt Cancer Research and Treatment Center He has treated thousands of cancer patients and undertaken hundreds of research studies as Medical Director for the Sarah Cannon Cancer Center.
This patient research was pivotal in perfecting this product.
From there, at one point to further my research, I worked closely with PearlPoint Cancer Support (formerly the Minnie Pearl Cancer Foundation). This organization provides trusted information and personalized resources to navigate cancer with confidence.
The following are comments made by Susan Hosbach, who was at the time, President and CEO of PearlPoint Cancer Support, regarding Dr. Steve’s Nutri Snax-PIZZA:
“You have a home run! It is so flavorful. I love this and could see myself snacking on it regularly. I believe it is the perfect blend for cancer patients, not overwhelming, just very, very tasty! Thanks so much for letting us be a ‘test tasting’ group.”
Warmest regards,
Susan
Susan Earl Hosbach, CFRE
Former President & CEO
PearlPoint Cancer Support


(L-R) Micki Slingerland, Dr. Steve Snodgrass, and Robert Hatch attends Center Stage at The Opry celebrating Minnie Pearl's 100th at The Grand Ole Opry on October 22, 2012 in Nashville, Tennessee.
In summary, we must never forget Protein Calorie Malnutrition (PCM), may affect any patient, but it has the most-dramatic effect in those with a malignancy. PCM is the most-common secondary diagnosis in cancer patients. This is an alarm that must be answered. PCM increases morbidity, mortality, complications, length of hospital stay, and hospital readmissions. In many cases, PCM may be avoided, and that should be the initial goal. The truth is we can perform the perfect operation, follow standards of care to the letter, apply the best available technology and all of it won’t matter if we lose the patient because they could not eat enough protein. We often overlook the basic things, as nutrition is at the very core of human existence-especially, protein. We no longer can allow this to happen. I recommend every cancer patient (in the presence of a family member), ask their caregivers this question: HOW MANY GRAMS OF PROTEIN DO I NEED TO EAT EVERYDAY? You should expect and deserve to know the answer, and then do everything in your power to meet that number.
BREAST CANCER
As a General Surgeon, so much of my training and practice involved cancer patients and meeting their very specific, individual needs. To give you an idea of a General Surgeon’s life and experience as it relates to cancer, here is a list of primary and metastatic malignancies where I have been called upon to surgically intervene: skin, head and neck, esophagus, thymus, mediastinum, lung, pleura, diaphragm, peritoneum, liver, pancreas, gall bladder, bile duct, stomach, small bowel, appendix, colorectal/anal, ovarian/Fallopian tube/uterine/cervical, leukemia/lymphoma, spleen, blood vessels, testicular/bladder/kidney/adrenal, muscle, bone, brain and spinal cord. This emphasizes and explains the “GENERAL,” in GENERAL SURGEON.
That being said, considering all my cancer cases, the majority involved breast cancer. From biopsy to lumpectomy to mastectomy, these patients, both male and female, became patients for life. For this reason, among others, I devoted special attention to this specific malignancy. Nutrition plays a key role in this disease. In addition to being linked to excess body fat and drinking alcohol, there are new clinical discoveries concerning breast cancer and how food may become a friend. Now, more than ever, it is of vital importance to make wise choices concerning nourishment for your body in this special time of need. These latest findings are exciting and something we all should know about because they give the patient some degree of power in the course of their disease. You control what you choose to eat and why. Clearly, there is evidence to support some foods are proving to be more beneficial than others.
Breast cancer is another one of the main reasons this product is made with soy protein. This is validated by findings published in the medical/surgical/oncology literature. From the Journal of the American Medical Association, JAMA, 2009, a published article titled Soy Food Intake and Breast Cancer Survival concluded: Among women with breast cancer, soy food consumption was significantly associated with decreased risk of death and recurrence. It did not appear to vary by menopausal status and was evident for women with ER-positive and ER-negative cancers and early and late-stage cancers.
Shu XO, Zheng Y, Cai H, et al. Soy Food Intake and Breast Cancer Survival. JAMA. 2009;302(22):2437-2443. doi:10.1001/jama.2009.1783
Additionally, the following conclusion was drawn in an article published in CANCER, 3/16/17 from the American Cancer Society: In this large, ethnically diverse cohort of women with breast cancer living in North America, a higher dietary intake of soy isoflavone was associated with a reduced all cause mortality. If anyone of the reported 3.5 million breast cancer patients living in this country, especially one of the 150,000 who has metastatic breast cancer would ask me why they should eat soy protein every day, my first response would simply be, “Why not?”
Disclaimer: No content on this site should ever be used as a substitute for direct medical advice from your doctor or other qualified clinicians.